Live
- 10 Tried-and-Tested Home Remedies for Toothaches
- Thila Taila Abhishekah Pooja to Lord Shaneswara
- Sudheer Babu’s ‘Harom Hara’ set to release on this auspicious day
- Priyanka Gandhi says BJP talking of 'tinkering' with Constitution with PM’s nod
- Vishwak Sen unveils gritty avatar as ‘Lankala Rathna’ in ‘Gangs of Godavari’ teaser
- ‘Kalki 2898 AD’ locks release date; film to entertain audience from June last week
- LS polls: PM Modi says BJP-NDA leading 2-0 after first two phases
- Plea in Madras HC seeks special polling arrangement for names 'missing' from Coimbatore voter list
- Ex CM KCR Bus tour on 4 th day
- Youth National Games 2024 kick-start in Delhi; over 5,000 athletes from 15 states vying for top honours
Just In
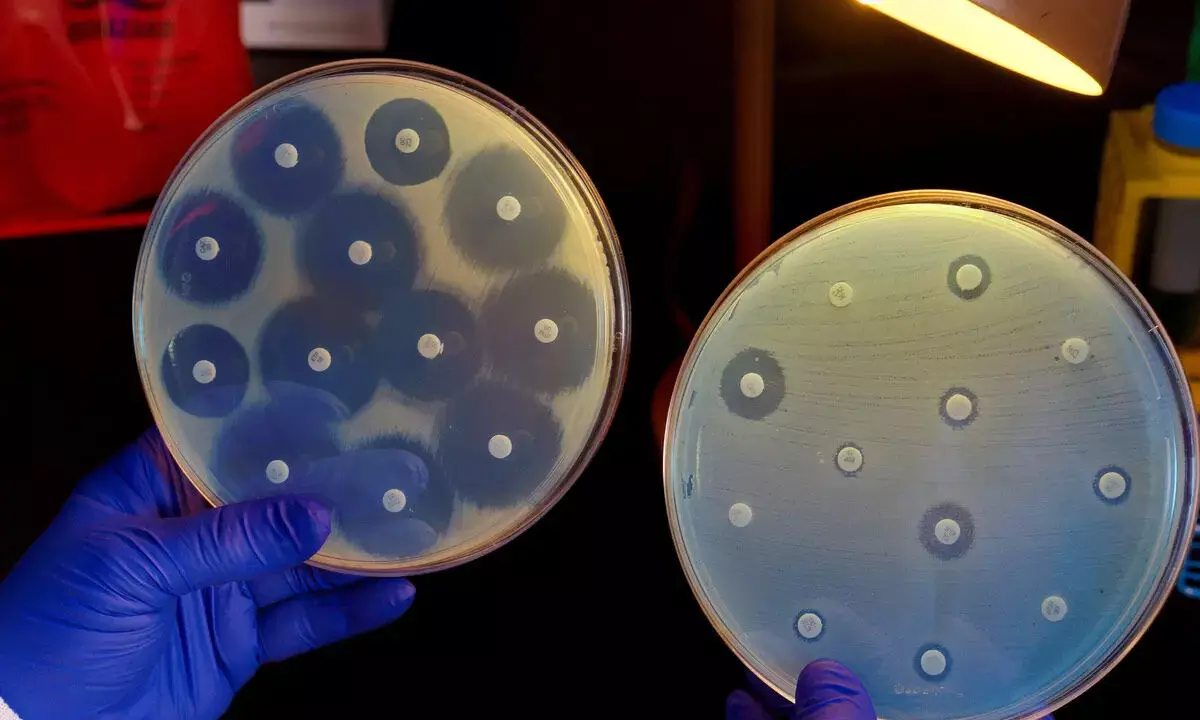
“What doesn’t kill me makes me stronger”, originally coined by Friedrich Nietzsche in 1888, is a perfect description of how bacteria develop antibiotic resistance
“What doesn’t kill me makes me stronger”, originally coined by Friedrich Nietzsche in 1888, is a perfect description of how bacteria develop antibiotic resistance. Contrary to a common belief, antibiotic resistance is not about your body becoming resistant to antibiotics. Resistance arises when bacteria are exposed to levels of antibiotics that don’t immediately kill them. They develop defences that prevent the same antibiotic from harming them in the future, even at higher doses.
Bacteria develop resistance to antibiotic treatment using four main methods:
1) Keep the antibiotic out. Bacteria are good at keeping unwanted molecules from getting inside: Gram-positive bacteria like Staphylococcus aureus have a thick cell wall enclosing a lipid membrane. Gram-negative bacteria, such as E. coli, are more difficult to kill as they have an additional outer membrane that acts as an extra barrier.
Bacteria are able to bring in the things they need to survive through these cell surfaces. Antibiotics can hijack these entry routes, but bacteria can modify the cell wall, cell membrane and entry proteins to block antibiotic penetration. For example, bacteria increase the thickness of the cell wall to resist antibiotics like vancomycin.
2. Expel the antibiotic if it gets in. Bacteria have machinery known as efflux pumps, which regurgitate unwanted molecules from within the bacteria: Bacteria can alter the pump so it is more effective at removing the antibiotic, or they can simply make more pumps. Resistance to macrolide antibiotics like erythromycin often involves the production of more efflux pumps.
3) Alter the antibiotic target: Antibiotics, like most other drugs, generally work by blocking the function of important enzymes within the bacteria. They specifically bind to the target like a key in a lock. If bacteria alter the target shape by changing the DNA/protein sequence, the antibiotic (key) can no longer bind to its target (lock). Resistance to a class of antibiotics known as fluoroquinolones (which includes ciprofloxacin) often occurs due to mutations of the enzyme targets.
4) Destroy or modify the antibiotic: Bacteria developed resistance to the original antibiotic, penicillin, by producing a protein that breaks apart the penicillin warhead. These enzymes have evolved to keep pace with even the most recent new and improved penicillin-like antibiotics. In response, drug developers have created molecules that specifically stop the enzyme from working, and dose these in combination with the antibiotic.
Another example of antibiotic modification is shown by resistance to a class of antibiotics called aminoglycosides. In this case, different types of enzymes chemically modify the structure of the aminoglycoside, such as the antibiotic tobramycin. Now, the key has been filed so that it no longer fits the lock.
(Mark Blaskovich, Professor, The University of Queensland, in The Conversation: How do bacteria actually become resistant to antibiotics?)

© 2024 Hyderabad Media House Limited/The Hans India. All rights reserved. Powered by hocalwire.com







