A question of life and death
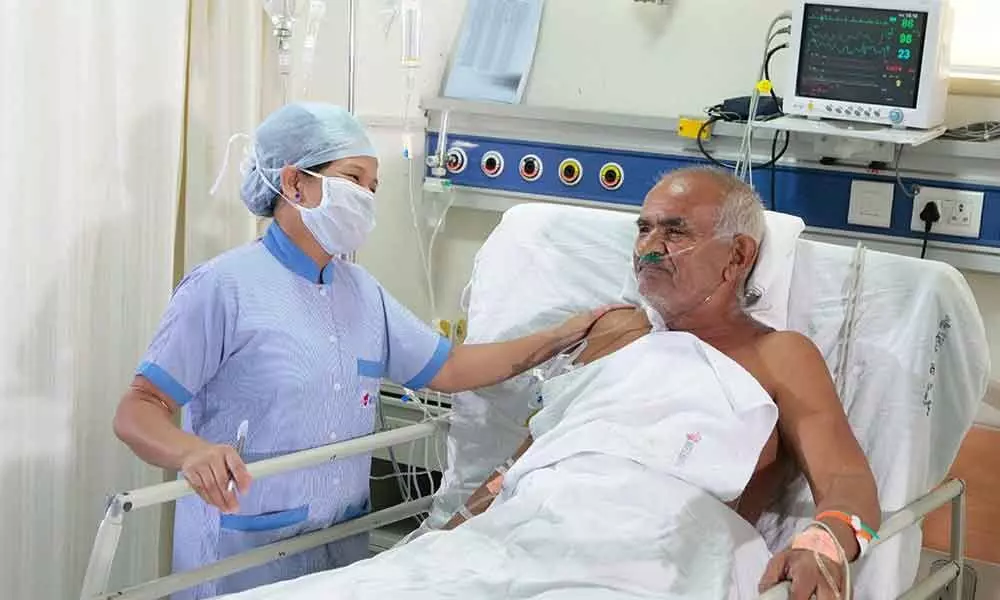
A question of life and death
Dying is an inevitable part of the life cycle. Everybody aspires to live a long life and die a painless death. But, too many of us have seen bad death, with lot of pain, suffering, depression and loneliness.
Dying is an inevitable part of the life cycle. Everybody aspires to live a long life and die a painless death. But, too many of us have seen bad death, with lot of pain, suffering, depression and loneliness. Although treatment for terminally-ill ailments like cancer is improved since last two decades, there is no change in the severe pain undergone, various hitches of hospitalisation and prolonged-illness and suffering near the end of life.
More people are dying today of chronic diseases, and the average person can expect to spend the last decade of his life being seriously ill and under constant medical treatment.
This is the adverse downside of extended life years: the life expectancy in 1960 was 40 years, today it is 72 years. Studies, however, have shown that end of life medical interventions are largely unnecessary and ineffective, as, of those who die in hospitals fully one-third will do so in ICUs and one fifth will have undergone redundant operations in the last month of their lives. Recent health science studies shows that pain relieving, quality care, interaction with family, near and dear are equally important if not more than the treatment itself during the end of life.
The Indian society places special value on treatments that prolong life – even for a few months – near the end of life. Prolonging life at any cost forcing terminally-ill patients into and out of hospitals with no value assigned to patient's preferences for pain relieving and healthy family interactions is reason behind the bad deaths. Though many studies have established that the quality of life of terminally-ill patients mostly depends on pain relieving, patient interactions with family members rather than prolonging life itself. Quality of life near the end of life differentiate good from bad death.
With so many diagnosed with terminal illnesses each year, as humans, we need to balance between quality of life and prolonged life itself. Part of living a good life is not living in fear - and living in fear of a long, drawn out, unpleasant, awful death is taking away a good quality of life.
There are many cases, where cancer patients are died just after 15 days of radiotherapy, which is unnecessary and painful. Treatments for terminal illnesses are non-curative by definition and so are likely to result in relatively small health gains when compared to other types of treatment. Such health gains often come at high cost and hence treatment of this type are less likely to meet cost-effectiveness threshold. Often, treatment of terminally-ill patients are breeding ground for corruption in terms of compelling unnecessary tests, surgeries and radiotherapy without any improvement in health.
In the name of extending life of terminally ill patients, the society is not only spending huge amount of money in ICUs and surgeries and radiotherapy etc without much improvement in health, but also forcing the patients to experience lot of pain, locked up in hospitals away from their families and eventually forced in to psychological and emotional depression. Moral dilemma of how to accommodate patient's interests like pain relieving, quality care,and life quality while extending the life is still unresolved. Relative value of life extensions for people with terminal illnesses like cancer needs to be addressed with the perspective of patients rather than a single motto of extending life at any cost.
Any major surgical operation with huge costs for terminally ill patients needs to cross a minimum cost-effectiveness threshold of extending life, normally of at least an additional 3 months. All end-of life major treatments for terminally-ill patients needs consider cost per Quality Adjusted Life Year (QALY) before deployment.If treatments are not crossing the threshold, the same efforts needs to place to enhance the quality of life.
Medical fraternity has to listen to patient's interests and needs. The medical establishment in India needs to initiate a dialogue on the subject so that we could adopt a more humane approach to the inevitability of death.
There are wide variety of medicines available now to decrease depression and anxiety, reduce pain and improve quality of life in patients with life-threatening cancer. The societal norms should encourage use of feel-good medicines instead of forcing painfulradiotherapy and other surgeries for terminally-ill patients.
Historically, indigenous cultures encouraged use of psilocybin and other hallucinogens as part of treating dying patients to induce heightened states of optimism under strict doctor's supervision.
The end-of-life treatment should focus on palliative care.Recent advances in palliative care make it highly effective in dealing with extreme pain and other suffering.
Issues like patient's physical comfort, pain-relieving, daily care, and emotional and spiritual health are key ingredients of treatment. Good interaction and emotional exchanges with family members, sufficient time and space for spiritual enlightenment, piece, sharing past experiences with sons and daughters and grandsons are all the more important than the medicine.
In terminal cases the medical fraternity should not regard death as a challenge but as a release, and should prepare their patient for good death.
(The author is a principal scientist and freelance columnist. Views expressed are personal)

















